- Published
- March 29, 2026
What Does a Defibrillator Do? How AEDs Save Lives During Cardiac Emergencies
What Is a Defibrillator? Definition and Purpose
A defibrillator is a medical device that delivers a controlled electrical shock to the heart to restore its normal rhythm during a life-threatening cardiac emergency. When a person experiences sudden cardiac arrest (SCA), the heart’s electrical system malfunctions, causing it to quiver chaotically instead of pumping blood. A defibrillator analyzes the heart’s rhythm, identifies the abnormality, and delivers a precise shock to reset the heartbeat. For a broader overview of all defibrillator types, see our complete guide to how defibrillators work.
Browse Response Ready’s complete collection of FDA-approved AEDs from all six manufacturers and find the right defibrillator for your needs. To learn more about staying compliant, read our AED compliance requirements.
Ready to find the right device? Learn how to compare all six FDA-approved defibrillator machines in our buying guide.
According to the American Heart Association, more than 350,000 out-of-hospital cardiac arrests occur in the United States every year. The survival rate without immediate intervention is approximately 10%. However, when a defibrillator is used within the first few minutes, survival rates can increase to 70% or higher. That makes understanding what a defibrillator does more than an academic exercise; it is knowledge that can genuinely save a life.
Response Ready, an authorized distributor of all six FDA-approved AED manufacturers in the U.S., has spent more than a decade helping schools, businesses, fitness centers, and families equip themselves with these life-saving devices. This guide explains the science behind defibrillation, how modern AEDs work, and why having one nearby is one of the most important safety decisions you can make.
How Does a Defibrillator Work? The Science of Defibrillation
A defibrillator works by sending a carefully measured electrical current through the heart muscle. This electrical pulse temporarily stops all cardiac electrical activity, giving the heart’s natural pacemaker (the sinoatrial node) an opportunity to regain control and resume a normal, coordinated rhythm. Think of it as pressing a “reset button” on a malfunctioning system.
The heart relies on electrical signals to coordinate each beat. During a normal heartbeat, the sinoatrial node sends an impulse that travels through the atria, passes through the atrioventricular node, and moves down into the ventricles. This coordinated wave of electricity causes the heart to contract in a precise sequence, pushing blood through the body.
During sudden cardiac arrest, this orderly process breaks down. The most common cause is ventricular fibrillation (VF), where the ventricles receive rapid, chaotic electrical signals and quiver uselessly instead of contracting. Another shockable rhythm is ventricular tachycardia (VT), where the ventricles beat too fast to pump blood effectively.
What Happens When the Shock Is Delivered
When a defibrillator delivers its shock, the electrical current passes through the chest and into the heart. The energy, measured in joules, is strong enough to momentarily depolarize all the heart muscle cells simultaneously. This brief pause in electrical activity creates a window for the sinoatrial node to resume generating normal impulses. If successful, the heart begins beating in a coordinated rhythm again, restoring blood flow to the brain and vital organs.
Modern AEDs typically deliver between 120 and 360 joules of energy, automatically adjusting the dose based on the patient’s impedance (the resistance of the body to electrical current). This ensures the shock is both effective and as safe as possible.
How Does an AED Analyze Heart Rhythms?
An Automated External Defibrillator (AED) uses sophisticated built-in algorithms to analyze the patient’s heart rhythm through adhesive electrode pads placed on the chest. These pads detect the heart’s electrical activity, much like a simplified electrocardiogram (ECG), and feed the data to the AED’s onboard computer.
The AED’s software evaluates several characteristics of the detected rhythm, including the rate, regularity, amplitude, and morphology of the electrical signal. Within seconds, the device determines whether the rhythm is “shockable” or “non-shockable.”
Shockable vs. Non-Shockable Rhythms
| Rhythm Type | Description | AED Action |
|---|---|---|
| Ventricular Fibrillation (VF) | Chaotic, disorganized electrical activity; heart quivers instead of pumping | Shock advised |
| Ventricular Tachycardia (VT) | Abnormally fast heart rate originating in the ventricles; often no pulse | Shock advised |
| Asystole | No detectable electrical activity (“flatline”) | No shock; continue CPR |
| Pulseless Electrical Activity (PEA) | Organized electrical rhythm but no effective pumping | No shock; continue CPR |
| Normal Sinus Rhythm | Healthy, coordinated heartbeat | No shock advised |
This automatic analysis is what makes AEDs safe for bystanders to use. The device will never deliver a shock to a heart that is beating normally. FDA-approved AEDs from manufacturers like Philips, ZOLL, HeartSine, Stryker/Physio-Control, Cardiac Science, and Defibtech have all been rigorously tested to ensure their algorithms correctly identify shockable rhythms with extremely high accuracy.

What Is the Difference Between an AED and a Manual Defibrillator?
An AED (Automated External Defibrillator) is a portable, user-friendly device designed for use by anyone, regardless of medical training. A manual defibrillator is a complex medical instrument used by paramedics, emergency physicians, and trained healthcare professionals in clinical settings. Both devices deliver electrical shocks to the heart, but they differ significantly in who operates them and how.
Key Differences at a Glance
| Feature | AED (Automated External Defibrillator) | Manual Defibrillator |
|---|---|---|
| Intended User | Bystanders, employees, teachers, coaches | Paramedics, doctors, nurses |
| Training Required | Minimal; voice-guided instructions | Extensive medical training |
| Rhythm Analysis | Automatic; device decides if shock is needed | Manual; operator reads ECG and decides |
| Energy Settings | Pre-set or auto-adjusted | Manually selected by operator |
| Portability | Lightweight (2-7 lbs), wall-mounted in public spaces | Larger, mounted on crash carts or ambulances |
| Cost | $1,400 – $2,900 | $10,000 – $35,000+ |
| Typical Location | Schools, offices, gyms, airports, homes | Hospitals, ambulances, emergency departments |
For a deeper comparison between these two types of devices, read our detailed guide on manual defibrillator vs. AED differences.
The most important takeaway is that AEDs are specifically designed so that anyone can use them in an emergency. Voice prompts walk the rescuer through every step, from placing the electrode pads to standing clear while the device analyzes the rhythm and delivers the shock.
Why Does Early Defibrillation Matter So Much?
Early defibrillation is the single most critical factor in surviving sudden cardiac arrest outside of a hospital. For every minute that passes without defibrillation, a person’s chance of survival decreases by approximately 7% to 10%. After 10 minutes without a shock, the odds of survival drop to near zero.
The average emergency medical services (EMS) response time in the United States is 7 to 14 minutes. In rural areas, it can exceed 20 minutes. This gap between cardiac arrest onset and professional help is exactly why public-access AEDs save lives. A bystander who can reach an AED and deliver a shock within 3 to 5 minutes gives the victim the best possible chance of survival.
The Chain of Survival
The American Heart Association’s Chain of Survival outlines five critical links for surviving out-of-hospital cardiac arrest:
- Early recognition and calling 911 to activate emergency services
- Early CPR to maintain blood flow to the brain and heart
- Early defibrillation to restore a normal heart rhythm
- Advanced emergency medical care provided by paramedics
- Post-cardiac arrest care at a hospital
Research published in medical journals consistently shows that communities with widespread AED access and bystander training see significantly higher survival rates. In locations where AEDs were available and used before EMS arrived, survival rates from ventricular fibrillation reached 38% or higher, compared to just 9% with CPR alone.

Where Should AEDs Be Placed?
AED placement should prioritize locations where large numbers of people gather and where the risk of cardiac arrest is elevated. Response Ready recommends the following locations as priorities for AED installation:
- Schools and universities: 16 states now mandate AEDs in schools, and student athletes face heightened risk during physical activity
- Gyms and fitness centers: Over 20 states require AEDs in fitness facilities due to exertion-related cardiac events
- Corporate offices and workplaces: With large employee populations spending 8+ hours daily, workplace AED programs protect your team
- Churches and community centers: Aging congregations are at elevated cardiac risk. Read our complete church AED program guide
- Airports, hotels, and public venues: High-traffic spaces where thousands pass through daily
- Homes: Approximately 70% of out-of-hospital cardiac arrests happen at home, making a home AED a wise investment for families with cardiac risk factors
Response Ready offers complete AED packages that include the device, a wall cabinet, signage, a first responder kit, and inspection materials, making it simple to set up a rescue-ready AED station in any location.
How to Choose the Right AED
Choosing the right AED depends on your specific environment, budget, and the level of training your staff or family members have completed. Response Ready carries all six FDA-approved AED brands, allowing customers to compare options side by side rather than being limited to a single manufacturer’s product line. If portability is a priority, our best portable defibrillators guide compares the lightest and most travel-friendly models.
Factors to Consider When Selecting an AED
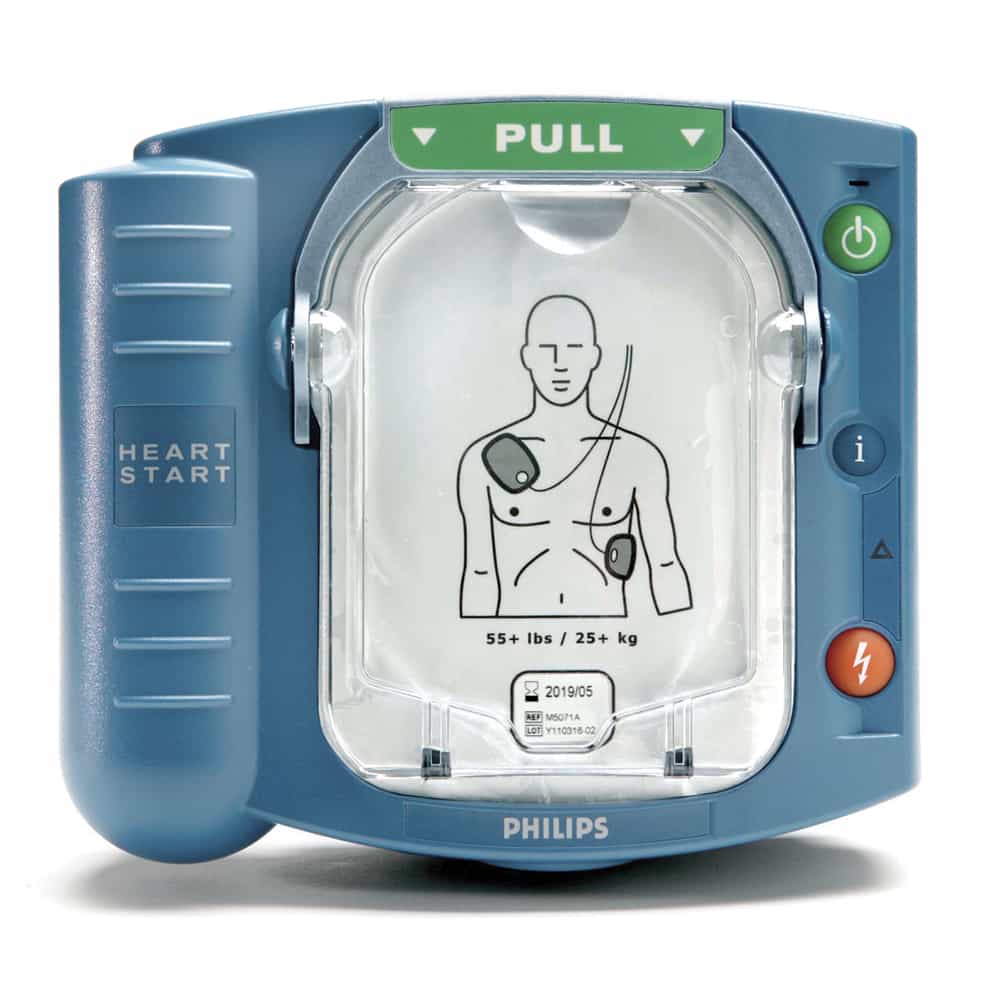
- Ease of use: Look for clear voice prompts and visual instructions. Models like the Philips HeartStart OnSite are popular for their intuitive, step-by-step guidance
- CPR feedback: Some AEDs, such as the ZOLL AED Plus, provide real-time CPR coaching to help rescuers maintain proper compression depth and rate
- Environment durability: Outdoor or industrial settings need devices with higher IP ratings for dust and water resistance
- Pediatric capability: If children are present, choose an AED with pediatric pads or a pediatric mode
- Total cost of ownership: Consider not just the purchase price but also battery and pad replacement costs over the device’s lifespan
- Warranty: Most FDA-approved AEDs carry 7 to 8 year warranties
For organizations that want the simplest possible setup, Response Ready’s AED rental program includes the device, all consumable replacements, maintenance management, and medical oversight for a low monthly fee.
Can Anyone Use an AED?
Yes. AEDs are specifically engineered so that any bystander, even someone with zero medical training, can use one effectively during a cardiac emergency. Every FDA-approved AED provides clear, step-by-step voice instructions that guide the rescuer through the entire process: turning on the device, placing the electrode pads, standing clear during analysis, and pressing the shock button if instructed.
All 50 U.S. states have Good Samaritan laws that provide legal protection for bystanders who use an AED in good faith during a cardiac emergency. You cannot be held liable for trying to save a life with an AED, and the device’s built-in safety features prevent it from delivering a shock to a heart that is beating normally.
While formal CPR and AED training is always recommended and builds confidence, it is not required to operate an AED. The device is designed to do the thinking for you.
Keeping Your AED Rescue-Ready
Owning an AED is only the first step. Maintaining it in rescue-ready condition ensures the device will perform when needed. Response Ready recommends the following practices:
- Monthly visual inspections: Check the status indicator light to confirm the AED has passed its self-test
- Track expiration dates: Electrode pads and batteries have expiration dates that must be monitored and replaced before they expire
- Store properly: Keep the AED in its designated wall cabinet in a visible, accessible location
- Use a management program: Response Ready’s AED Total Solution program automates compliance tracking, sends expiration reminders, and provides medical oversight
For a comprehensive guide to keeping your device in top condition, read our AED maintenance checklist.
Frequently Asked Questions About Defibrillators
What does a defibrillator do to the heart?
A defibrillator delivers a controlled electrical shock that temporarily stops all electrical activity in the heart. This brief pause allows the heart’s natural pacemaker, the sinoatrial node, to regain control and restart a normal, coordinated rhythm. The shock does not “start” a stopped heart; it resets a heart that is beating chaotically.
Can a defibrillator restart a heart that has completely stopped?
No. A defibrillator is designed to treat abnormal heart rhythms like ventricular fibrillation and ventricular tachycardia. If the heart has completely stopped (asystole or “flatline”), a defibrillator will not deliver a shock. In that situation, CPR and advanced medical interventions are needed. For a detailed comparison, see our guide to the key differences between defibrillators and pacemakers.
Is it safe for an untrained person to use an AED?
Yes. AEDs are designed for use by anyone. They provide voice-guided instructions and will only deliver a shock when the device detects a shockable rhythm. Good Samaritan laws in all 50 states protect bystanders who use an AED in good faith during an emergency.
How much does an AED cost?
FDA-approved AEDs typically range from $1,400 to $2,900 depending on the manufacturer, model, and included accessories. Response Ready offers value packages that bundle the AED with a cabinet, signage, and first responder kit at competitive prices. Monthly rental programs start at $45 per month.
How often should an AED be inspected?
AEDs should receive a brief visual inspection at least once per month. Check the status indicator to confirm the device has passed its self-test, and verify that electrode pads and batteries have not expired. A comprehensive AED management program can automate these checks.
Do AEDs work on children?
Yes. Most AEDs can be used on children by switching to pediatric electrode pads or activating a pediatric mode that reduces the energy delivered. For infants and children under 8 years old or weighing less than 55 pounds, pediatric pads are recommended. If pediatric pads are not available, adult pads can still be used in a life-threatening emergency.
Disclaimer for information purposes only:
The information provided on this website is intended for general educational and informational purposes only. It is not medical advice and should not be used as a substitute for professional diagnosis, treatment, or care. Always consult a qualified healthcare or medical professional regarding any health-related questions or concerns.
While we strive to ensure the information shared is accurate and up to date, no guarantees are made regarding completeness, accuracy, or applicability to any individual situation. Use of this content is at the reader’s sole discretion and risk.
This website is part of the Response Ready family of emergency preparedness and training resources, including CPR & first aid training and compliance services, AED sales and program support, AED program management software, and medical oversight solutions provided through our affiliated platforms:
• CPR1.com
• AEDLeader.com
• AEDTotalSolution.com
• MDSIMedical.com
By accessing or using this website, you agree to release, indemnify, and hold harmless the website owners, authors, contributors, and affiliated entities from any claims, losses, damages, or liabilities arising from the use or reliance on the information presented.