- Published
- March 27, 2026
Defibrillator vs Pacemaker - What's the Difference?
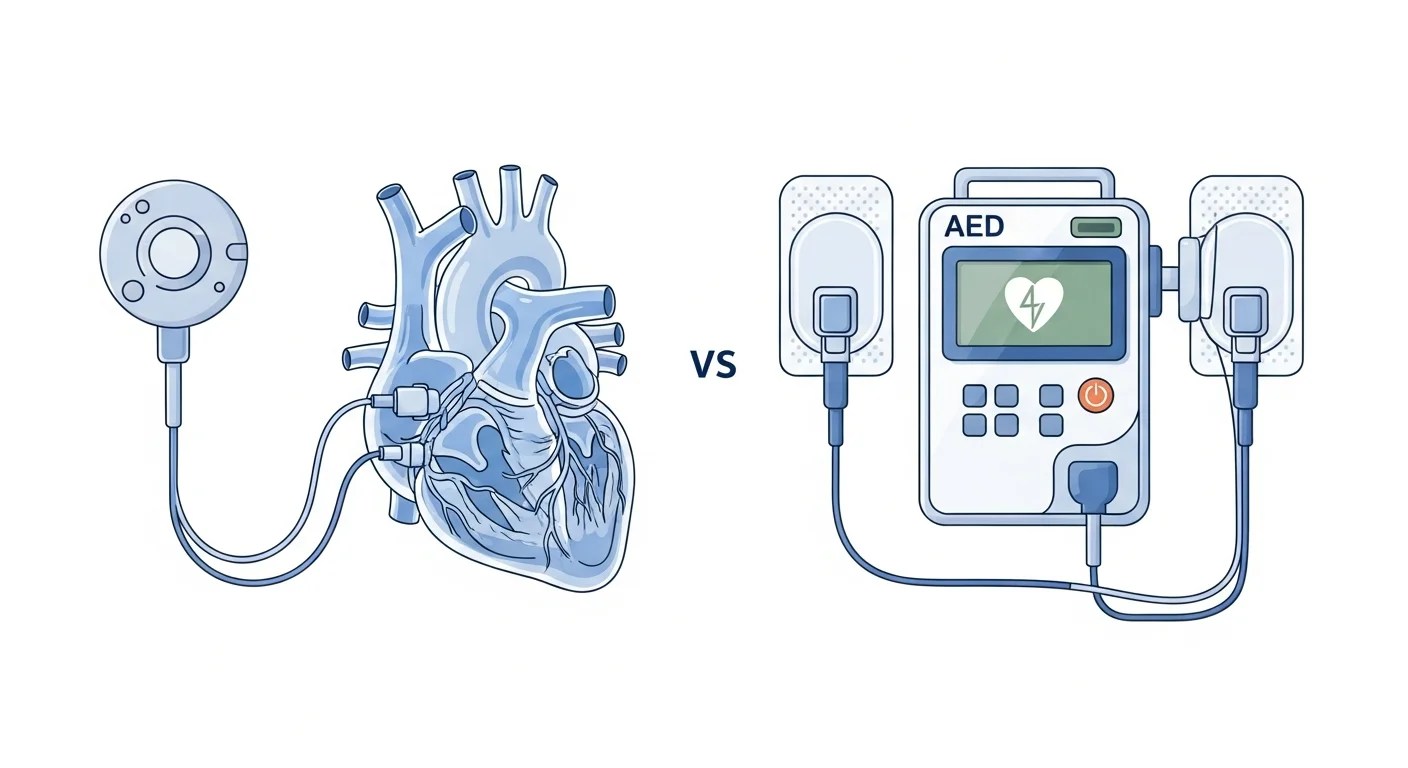
What Is the Difference Between a Pacemaker and a Defibrillator?
Is a defibrillator the same as a pacemaker? Many people ask this question, and the answer is no. While both devices use electrical signals to support heart function, they serve fundamentally different purposes. A pacemaker keeps a slow or irregular heartbeat steady, while a defibrillator delivers a life-saving shock to reset a dangerously fast or chaotic heart rhythm. Response Ready, an authorized distributor of all six FDA-approved AED manufacturers, explains the key differences so you can make informed decisions about cardiac safety.
Browse FDA-approved AEDs from all six manufacturers at Response Ready.
Each year, more than 356,000 people in the United States experience out-of-hospital sudden cardiac arrest (SCA), according to the American Heart Association. Survival rates improve dramatically when a defibrillator is used within the first few minutes. Pacemakers, on the other hand, are long-term implanted devices that help millions of Americans maintain a healthy heart rhythm every day. Both devices play critical roles in cardiac care, yet many people confuse them or assume they do the same thing.
How Does a Pacemaker Work?
A pacemaker is a small, battery-powered device implanted under the skin near the collarbone. It connects to the heart through thin wires called leads and continuously monitors the heartbeat. When the heart beats too slowly (a condition called bradycardia) or skips a beat, the pacemaker sends gentle electrical pulses to restore a steady rhythm.
Pacemakers treat conditions where the heart’s natural electrical system fails to maintain a normal rate. Common conditions that require a pacemaker include:
- Bradycardia: A resting heart rate below 60 beats per minute that causes symptoms such as fatigue, dizziness, or fainting
- Heart block: A delay or disruption in the electrical signals that coordinate heartbeats between the upper and lower chambers
- Sick sinus syndrome: A malfunction in the heart’s natural pacemaker (the sinoatrial node) that causes alternating slow and fast rhythms
- Heart failure: Certain types of heart failure benefit from cardiac resynchronization therapy (CRT), which uses a specialized pacemaker to coordinate the heart’s chambers
Modern pacemakers are about the size of a large coin and typically last 7 to 15 years before the battery needs replacement. Some newer models are leadless, meaning they are placed directly inside the heart without external wires.
How Does a Defibrillator Work?
A defibrillator monitors heart rhythm and delivers a controlled electrical shock when it detects a life-threatening arrhythmia. Unlike the gentle pulses of a pacemaker, a defibrillator shock is strong enough to reset the heart’s electrical activity entirely, allowing a normal rhythm to resume.
Defibrillators are designed to treat two specific life-threatening rhythms:
- Ventricular fibrillation (V-fib): The heart quivers chaotically instead of pumping blood
- Pulseless ventricular tachycardia (V-tach): The heart beats so fast that it cannot fill with blood between contractions
Both conditions cause sudden cardiac arrest, which is fatal within minutes without treatment. A defibrillator analyzes the heart’s rhythm and delivers a shock only when one of these dangerous patterns is detected.

Read Response Ready’s step-by-step AED guide for cardiac emergencies.
Implantable vs. External Defibrillators
Defibrillators come in two main categories: implantable devices that stay inside the body and external devices designed for emergency use by bystanders or medical professionals.
Implantable Cardioverter-Defibrillator (ICD)
An implantable cardioverter-defibrillator is a small device placed under the skin, similar to a pacemaker. It connects to the heart with leads and continuously monitors heart rhythm. If the ICD detects ventricular fibrillation or dangerous tachycardia, it delivers an internal shock to restore normal rhythm. Many modern ICDs also include pacemaker functionality, allowing them to treat both slow and fast heart rhythms in a single device.
Doctors typically recommend an ICD for patients who have survived a cardiac arrest, have a history of dangerous arrhythmias, or have certain heart conditions that place them at high risk for sudden cardiac death.
Automated External Defibrillator (AED)
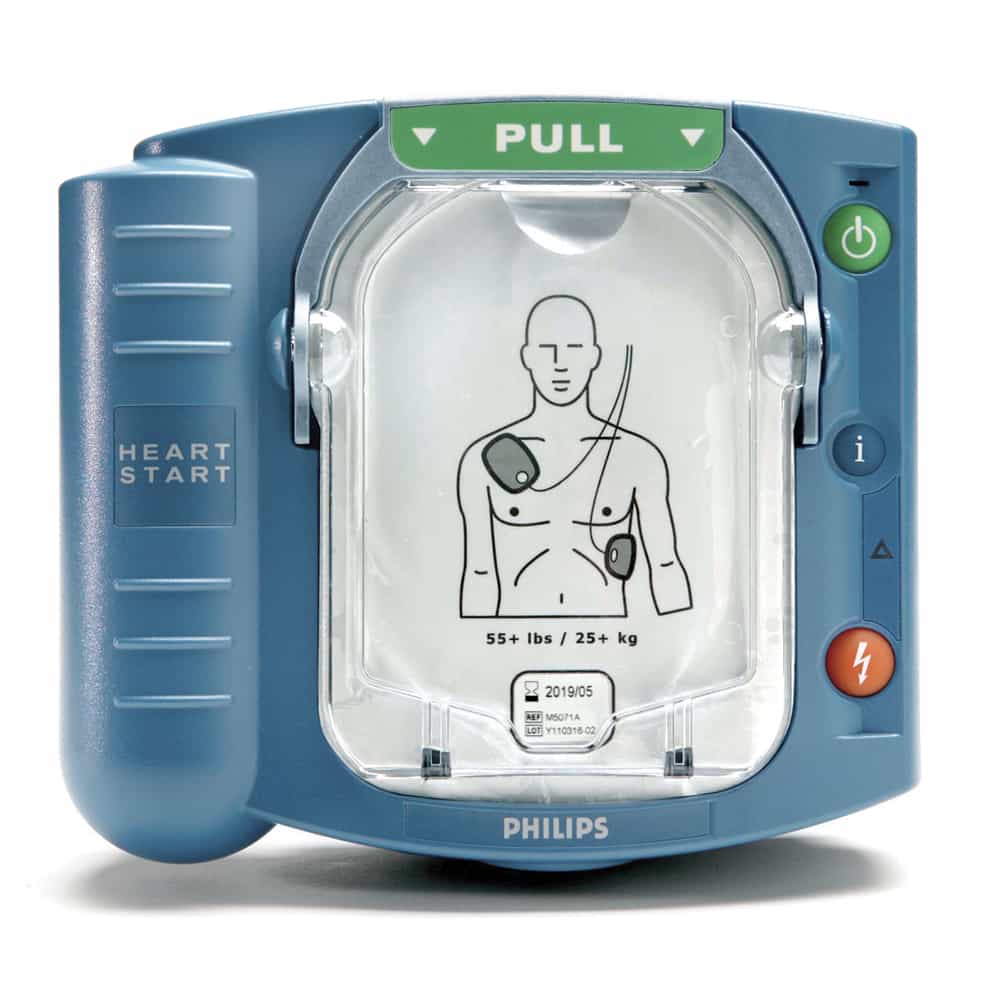
An automated external defibrillator is a portable device designed for use by anyone, including people with no medical training. AEDs are found in schools, offices, airports, gyms, churches, and other public spaces. When someone collapses from sudden cardiac arrest, a bystander can apply the AED pads to the person’s chest, and the device automatically analyzes the heart rhythm. If a shockable rhythm is detected, the AED delivers the shock through voice-guided instructions.
AEDs are specifically designed for sudden cardiac arrest emergencies that happen outside a hospital. They bridge the gap between the moment of collapse and the arrival of emergency medical services. According to the American Heart Association, using an AED within the first three to five minutes of cardiac arrest can increase survival rates to 70% or higher.
Manual Defibrillators
Manual defibrillators are used by trained medical professionals in hospitals and ambulances. Unlike AEDs, manual defibrillators require the operator to interpret the heart rhythm and decide when to deliver a shock. They offer more control over energy levels and timing, but they require specialized training to operate safely.
Defibrillator vs. Pacemaker: Side-by-Side Comparison
The following table summarizes the key differences between a pacemaker and a defibrillator, covering function, purpose, and common use cases.
| Feature | Pacemaker | Defibrillator (ICD/AED) |
|---|---|---|
| Primary function | Sends gentle electrical pulses to maintain a steady heartbeat | Delivers a strong shock to reset a dangerous heart rhythm |
| Treats | Bradycardia, heart block, sick sinus syndrome | Ventricular fibrillation, ventricular tachycardia, sudden cardiac arrest |
| Type of electrical signal | Low-energy pacing pulses | High-energy defibrillation shocks |
| When it activates | When the heart beats too slowly or irregularly | When a life-threatening arrhythmia is detected |
| Implanted or external | Implanted only | Implanted (ICD) or external (AED) |
| Who operates it | Functions automatically after surgical implantation | ICD: automatic; AED: bystander or first responder |
| Typical battery life | 7 to 15 years | ICD: 5 to 7 years; AED: 2 to 5 years (standby) |
| Can they coexist? | Yes, combination ICD/pacemaker devices are common | Yes, many ICDs include built-in pacemaker functions |
Who Needs a Pacemaker vs. a Defibrillator?
The type of heart rhythm problem determines which device a cardiologist will recommend. A pacemaker is the right choice for patients whose hearts beat too slowly or inconsistently. A defibrillator is prescribed for patients at risk of sudden cardiac arrest from dangerously fast or chaotic rhythms.
Candidates for a Pacemaker
- People diagnosed with symptomatic bradycardia
- Patients with second-degree or third-degree heart block
- Individuals with sick sinus syndrome
- Heart failure patients who qualify for cardiac resynchronization therapy
- People who experience frequent fainting due to slow heart rhythms
Candidates for an Implantable Defibrillator (ICD)
- Survivors of sudden cardiac arrest
- Patients with a history of sustained ventricular tachycardia
- Individuals with a severely reduced ejection fraction (typically below 35%)
- People with genetic conditions such as Brugada syndrome, long QT syndrome, or hypertrophic cardiomyopathy
- Patients with dilated cardiomyopathy or ischemic heart disease at high risk for sudden death
Some patients need both pacemaker and defibrillator functions. Combination devices that integrate ICD and pacemaker capabilities are widely used in modern cardiology practice.
Learn more about how defibrillators work and why they matter in cardiac emergencies.
Common Misconceptions About Pacemakers and Defibrillators
Confusion about these two devices is widespread. Here are the most common misconceptions, along with the facts.
Misconception 1: A pacemaker can restart a stopped heart
A pacemaker cannot restart a heart that has stopped beating entirely. It only works when there is some existing electrical activity to support. Restarting a heart in cardiac arrest requires a defibrillator shock, combined with CPR, to restore a viable rhythm.
Misconception 2: A defibrillator and pacemaker are the same thing
Is a defibrillator and pacemaker the same thing? No. While both devices interact with the heart’s electrical system, they serve opposite purposes. A pacemaker speeds up a slow heart. A defibrillator resets a dangerously fast or chaotic heart. Some devices combine both functions, but the underlying technologies are distinct.
Misconception 3: Only doctors can use a defibrillator
Automated external defibrillators are specifically designed for use by untrained bystanders. AEDs provide step-by-step voice instructions and will not deliver a shock unless the device confirms a shockable rhythm. No medical training is required to operate an AED safely, though CPR and AED training builds confidence and improves response time.
Misconception 4: You cannot touch someone while a defibrillator is in use
This is partially true. Bystanders should not touch the person during the moment the AED delivers its shock, as the electrical current could transfer. However, between shocks, it is safe and necessary to perform CPR. AEDs provide clear audio prompts that tell rescuers when to stand clear and when to resume chest compressions.
Misconception 5: People with pacemakers cannot be near AEDs
AEDs can be used safely on a person who has an implanted pacemaker. The AED pads should be placed at least one inch away from the pacemaker site (usually a visible bump under the skin near the collarbone). The AED will still analyze the heart rhythm accurately and deliver a shock if needed.
Why AED Access Matters for Every Organization
While pacemakers and ICDs are medical devices that require surgical implantation and a cardiologist’s oversight, AEDs are community safety tools that anyone can purchase and deploy. Sudden cardiac arrest does not discriminate by age, fitness level, or health history. It can happen to anyone, anywhere, at any time.
Organizations such as schools, workplaces, fitness centers, churches, and public venues have a responsibility to provide rapid access to defibrillation. Having an AED device on-site dramatically increases the chance of survival when every second counts. Response Ready carries AEDs from all six FDA-approved manufacturers, including Philips, ZOLL, HeartSine, Stryker/Physio-Control, Cardiac Science, and Defibtech, making it simple to find the right device for any environment.
Explore AED options from all six FDA-approved brands at Response Ready.
Frequently Asked Questions
What is the main difference between a pacemaker and a defibrillator?
A pacemaker sends low-energy electrical pulses to keep a slow heart beating at a steady rate. A defibrillator delivers a high-energy shock to reset a dangerously fast or chaotic heart rhythm. Pacemakers treat bradycardia, while defibrillators treat ventricular fibrillation and ventricular tachycardia.
Can a person have both a pacemaker and a defibrillator?
Yes. Many patients benefit from combination devices that include both pacemaker and ICD functions in a single implant. These devices can pace a slow heart and deliver a shock if a life-threatening arrhythmia occurs.
Do you need medical training to use an AED?
No. Automated external defibrillators are designed for use by anyone, including bystanders with no medical background. AEDs provide voice-guided instructions and only deliver a shock when the device detects a shockable rhythm. However, CPR and AED training from a certified provider improves confidence and response speed.
Can an AED be used on someone who has a pacemaker?
Yes. AEDs work safely on people with implanted pacemakers. Place the AED pads at least one inch away from the pacemaker (a small bump usually visible near the collarbone). The AED will still accurately analyze the heart rhythm and shock if necessary.
Does a pacemaker prevent sudden cardiac arrest?
A pacemaker alone does not prevent sudden cardiac arrest caused by ventricular fibrillation or tachycardia. Pacemakers address slow heart rhythms. To protect against sudden cardiac arrest from fast arrhythmias, an implantable cardioverter-defibrillator or access to an external AED is needed.
How long do pacemakers and defibrillators last?
Pacemaker batteries typically last 7 to 15 years, depending on usage and device settings. Implantable defibrillator batteries last approximately 5 to 7 years. AED batteries in standby mode last 2 to 5 years, depending on the manufacturer and model. Learn more about AED battery life and replacement costs.
Is a defibrillator and pacemaker the same thing?
No, a defibrillator and pacemaker are not the same thing. A pacemaker is an implanted device that sends gentle electrical pulses to keep a slow heartbeat steady. A defibrillator delivers a powerful shock to reset a dangerously fast or chaotic heart rhythm during cardiac arrest. They treat opposite types of heart rhythm problems.
What is the difference between a pacemaker and a defibrillator?
The main difference is their purpose. A pacemaker treats hearts that beat too slowly by providing steady electrical pulses. A defibrillator treats hearts that beat too fast or chaotically by delivering a strong shock to restore normal rhythm. Pacemakers are always implanted, while defibrillators can be implanted (ICD) or portable external devices (AED) used in emergencies.
Disclaimer for information purposes only:
The information provided on this website is intended for general educational and informational purposes only. It is not medical advice and should not be used as a substitute for professional diagnosis, treatment, or care. Always consult a qualified healthcare or medical professional regarding any health-related questions or concerns.
While we strive to ensure the information shared is accurate and up to date, no guarantees are made regarding completeness, accuracy, or applicability to any individual situation. Use of this content is at the reader’s sole discretion and risk.
This website is part of the Response Ready family of emergency preparedness and training resources, including CPR & first aid training and compliance services, AED sales and program support, AED program management software, and medical oversight solutions provided through our affiliated platforms:
• CPR1.com
• AEDLeader.com
• AEDTotalSolution.com
• MDSIMedical.com
By accessing or using this website, you agree to release, indemnify, and hold harmless the website owners, authors, contributors, and affiliated entities from any claims, losses, damages, or liabilities arising from the use or reliance on the information presented.